Covid-19 vaccines – a closer look
THE DEVELOPMENT and production of effective vaccines to prevent Covid-19 has been unprecedented. How has this been possible? asks professor Deborah Briggs.
Over coming weeks the virologist will take a closer look at all of the vaccines on offer, starting here with Oxford/AstraZeneca. Her next article will look at the data that has been published for the Covid-19 vaccine developed and produced by Pfizer.
The main reason is that researchers in today’s world have access to modern molecular techniques and procedures that were not available even a decade ago.
As a comparison, consider how technology associated with the travel industry has changed in the past few decades. For example, in the early 1800’s it took my own ancestors more than eight weeks to emigrate from Scotland to the wilderness of Canada and yet today, I can make that same journey in about eight hours by airplane.
In short, researchers in today’s modern laboratories have acquired the knowledge and technology to examine the tiniest components of viruses and to determine which of those components will produce the best immune response needed to prevent disease.
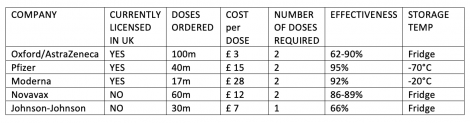
There are currently three Covid-19 vaccines licensed for use in the UK. Additionally, the UK government has put in advance orders for two additional Covid-19 vaccines that are still in the pipeline and are expected to be licensed in the UK sometime before the end of this year.
It may be of interest to understand a bit more information about each of the five vaccines that are currently available or will be available in the coming months.
Below I will discuss the published information/data detailing the effectiveness of the Oxford/AstraZeneca vaccine:
Become a member of Shetland News
The Oxford/AstraZeneca vaccine was developed at Oxford University with financial support from several institutions including the pharmaceutical company AstraZeneca.
The technology used to create this vaccine is different from many traditionally produced vaccines in how it alerts our immune system to respond and develop immunity to infection from the virus that causes Covid-19.
Older vaccine technology involves using a piece or even the whole virus to create a vaccine. Scientists ‘kill’ or inactivate that infectious virus, usually with chemicals. It is that ‘killed’ virus that constitutes the backbone of the older vaccines that create immunity.
The advanced vaccine technology that was used to develop many of the new Covid-19 vaccines skips a step and provides the information needed to create a vaccine directly to a patient’s immune system. From that information, our immune system produces antibodies that will attack the virus causing Covid-19 if and when we are exposed.
More information on the different types of technology used to make vaccines can be found on the Oxford Vaccine website.
In December 2020, the Oxford vaccine group published their much-awaited data from four large clinical trials conducted in human volunteers in the UK, South Africa, and Brazil. The results showed that the overall vaccine effectiveness after two doses of the Oxford AstraZeneca vaccine averaged 70 per cent.
Hospitalisations of patients for Covid related symptoms were significantly reduced in the vaccine group compared to the control group even after one dose of vaccine.
For example, two out of 12,021 patients that received one dose of AstraZeneca vaccine were hospitalised for Covid-19 compared to six out of 11,724 patients that did not receive the AstraZeneca vaccine.
After two doses of the AstraZeneca vaccine, the researchers reported that no patients were hospitalised in the subjects enrolled in the clinical trials. The full paper can be downloaded here.
We have been hearing an increasing amount of rather alarming news about how the virus that causes Covid-19 is changing over time and new viral variants are being identified, for example the variants recently identified in the UK, South Africa and Brazil.
Initial information from the Oxford AstraZeneca team indicates that their vaccine will still be effective against the new variants that have been identified. The situation about evolving viral variants is being closely monitored and more detailed information about the effectiveness of the AstraZeneca vaccine against the South African variant is expected to be released next week.
It is important to understand that many viruses change over time and this is a normal occurrence as viruses spread from person to person.
The virus that is probably the most famous for changing from year to year is the influenza virus. In fact, there are specific laboratories situated throughout the world that continually collect and analyse circulating influenza viruses to determine how the vaccines produced to prevent influenza need to be adjusted each year.
The genetic makeup of the collected influenza viruses are reported to a group of experts under the auspices of the World Health Organisation. This group of influenza experts examines the genetic code of the circulating influenza viruses from around the world and from that information, will determine how influenza vaccines need to be adjusted each year to provide continual protection.
This same procedure is in all likelihood what will happen with the coronaviruses that belong to the group causing the disease that we know as Covid-19.
The good news is that the new technology that has been used to develop the Covid-19 vaccines can be adjusted in a short amount of time to include changes that occur in the virus and thus will be able to continue to provide the best immunity possible.
Professor Deborah Briggs has served as an expert to the World Health Organisation in the field of rabies prevention. She has provided expertise in the field of vaccine production and clinical trials for major pharmaceutical companies and continues to teach an online graduate level course in Global Public Health for Kansas State University. She lives in Bridge End, Burra.
Also from Deborah Briggs:
‘Stay positive and test negative’ – the latest on the race to end the Covid-19 pandemic
Become a member of Shetland News
Shetland News is asking its readers to consider paying for membership to get additional perks:
- Removal of third-party ads;
- Bookmark posts to read later;
- Exclusive curated weekly newsletter;
- Hide membership messages;
- Comments open for discussion.
If you appreciate what we do and feel strongly about impartial local journalism, then please become a member of Shetland News by either making a single payment, or setting up a monthly, quarterly or yearly subscription.